In extensive deep burns the wound must be closed by autologous skin graft. Due to the limitation of the donor site, adequate skin grafts remain a significant difficulty. The technique to expend harvested skin graft was presented by Mr. Cicero Parker Meek1 from the University of South Carolina Aiken (USCA), USA in 1958. But the technique was complicated so after Tanner et al.,2 presented the mesh skin graft technique in 1964, the Meek technique was discontinued. In 1993, the modified Meek technique was reintroduced and it was claimed to be superior to the mesh skin grafting technique and at present is used by many burn centers worldwide.3 The Mesh graft technique creates perforations then stretches the skin out while the modified Meek technique cuts the skin into small square pieces and stretches these out, and they can be further expanded as needed. The modified Meek technique was introduced in Thailand in 2015 and we had the opportunity to perform this technique on two patients with extensive deep burn wounds.
A male patient from Thailand, aged 50 years, had a history of underlying hypertension and severe dependence on EtOH. He was injured by 22,000 volts of high electricity. He was conscious during the transfer to Bangkok Hospital headquarters from the initial hospital where he had been treated. He was diagnosed with a high voltage electrical injury, with burns to 55% of his total body surface area (TBSA), many parts of the wounds were considered deep tissue burns and he had suffered an inhalation injury. Post treatment, he underwent sequential burn debridement by sharp instruments, and hydrosurgery (Versajet).
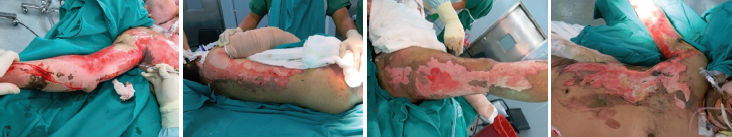
Figure 1: Day1.
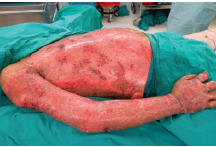
Figure 2: Day47.
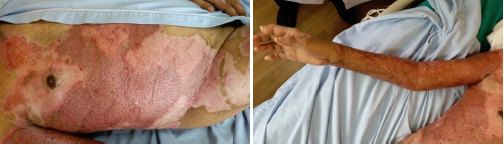
Figure 3: Day78.
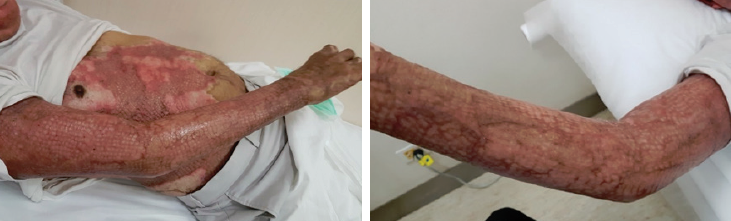
Figure 4: Day110, patient at OPD.
A 41-year old male from South Asia had 80%TBSA burns with an inhalation injury. He had initial treatment for his burns at a local hospital then was referred to Bangkok Hospital headquarters. On arrival, he presented with significant burns to the majority of his body, with the exception of his scalp, some sections of his abdomen and as well as minor area of both legs. The mortality rate is 79% in the age group of 40-50, with 71-80% TBSA burns also presenting an with inhalation injury.4 We used the modified baux score to predict the burn mortality rate in this study.5
After meticulous supportive treatment, he underwent and escharotomy of both arms and sequential debridement of the wounds with sharp instruments and hydrosurgery (versajet).
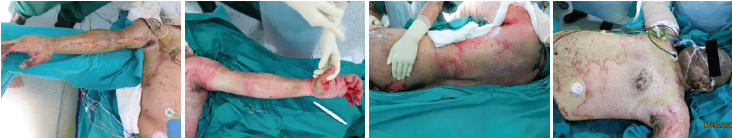
Figure 1: Arrival.
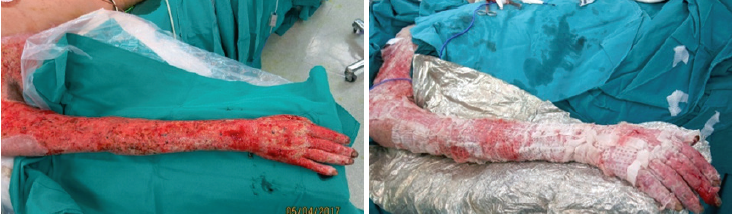
Figure 2: 30 day at the 1st graft.
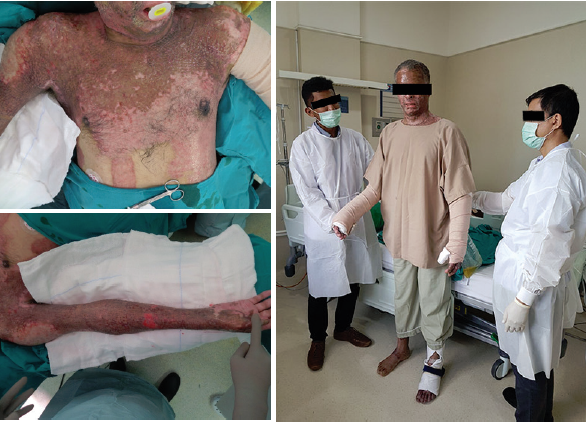
Figure 3: At 12 weeks.
In cases of patients with significant deep tissue burns, finding an adequate donor skin site is often problematic. The mesh technique that was introduced by Tanner et al.,2 can moderately reduce this issue. We find that if we use 1:1.5 mesh, the graft can cover only the wound just a little bit more than donor site, not 1.5 times. If we use 1:3 mesh we must use an intermediate thickness graft such as 0.018 inch, which for a prolonged illness burn patient, the donor site will heal over a much longer time period than usual. It may take 1-2 months to heal and there is likely to be a scar.
We used 1:4 expansion gauze and 0.014-inch thickness modified Meek skin grafting. It was shown that the graft can cover the wound 4 times more than the donor site. In addition, we found that we could use a small limited donor skin graft to cover a large deep burn wound area. The donor site healed within 1 month and the grafted area healed in about 2 weeks. The graft took about 90% with minimal infection and the area that was lost due to infection were only individual micro stamps and not the whole sheath as mesh graft. The risk of infection, whether lower or higher, cannot be evaluated here because of the few number of cases. Lastly, in our opinion, the late scar formation is comparable with conventional mesh shin grafting.
Meek technique skin grafting can be an alternative treatment for severe burn patients and is superior to conventional mesh skin grating as less area is required from the donor site. The technique provided a rapid and efficient surgical grafting for wound coverage compared to the conventional approach. Overall, it helped to increase the percentage of graft take and decreased the length of hospitalization stay. However, one disadvantage to take into account is the high cost of the treatment.
None declared.